Understanding Nervous System Regulation in Nerve Recovery
Nervous system regulation refers to the body’s ability to maintain balanced neural signaling. In addition, it supports adaptive stress responses and overall physiological stability across multiple systems.
In the context of nerve recovery, the nervous system regulation influences signaling sensitivity, inflammatory behavior, muscular tension, and autonomic balance. When regulation remains stable, neural communication becomes more efficient and less reactive. As a result, the internal environment becomes more supportive of repair readiness. As a result, the internal environment becomes more supportive of repair readiness and functional restoration.
Rather than focusing on symptoms alone, this module explores how regulatory mechanisms influence nerve behavior over time. It explains how stress load, emotional signaling, autonomic function, and biological rhythms influence neural stability and recovery capacity. Furthermore, it explains how regulatory balance supports long-term resilience.
Through this education layer, you will understand how Neural regulation operates, why dysregulation develops, and how regulatory balance supports long-term nerve health resilience.
Consequently, regulatory stability becomes essential for long-term recovery readiness. Therefore, understanding regulatory mechanisms becomes foundational within nerve recovery education.
What Is Nervous System regulation?
Nervous System regulation describes how the body stabilizes neural activity. It also regulates stress responses and autonomic function. It ensures that activation and recovery cycles remain balanced rather than chronically elevated or suppressed. As a result, physiological systems can maintain adaptive flexibility under stress.
The nervous system constantly interprets signals from the external environment. It also evaluates internal physiological signals. It evaluates safety, stress load, metabolic demand, and emotional input. Based on this interpretation, it adjusts heart rate, breathing patterns, muscle tone, and inflammatory signaling. In turn, this adaptive signaling helps stabilize internal recovery conditions.
When regulation functions efficiently, the body transitions smoothly between activation and restoration states. However, when regulatory capacity becomes overwhelmed, dysregulation may develop.
This shift does not occur instantly. Instead, it reflects cumulative biological stress, nervous system overload, and reduced adaptive flexibility over time.
The Biology of Nervous System regulation
Notably, autonomic signaling operates continuously in the background.
Importantly, autonomic regulation is rooted in autonomic nervous system function. Additionally, autonomic signaling supports recovery processes across multiple body systems. This system operates largely outside conscious control and governs survival-critical processes.
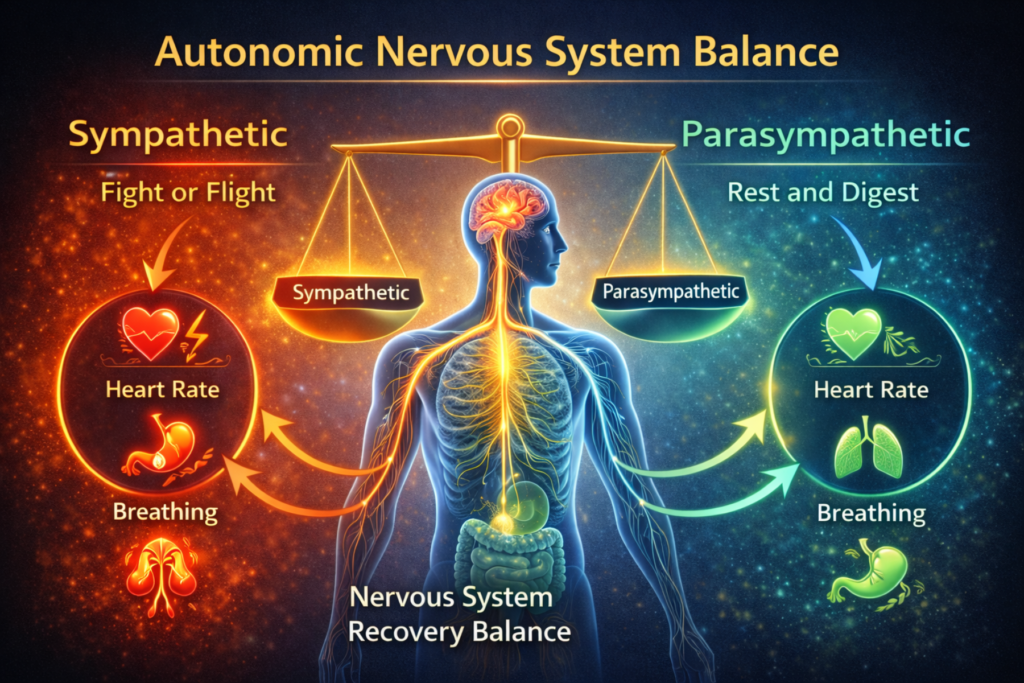
It consists of two primary branches:
- Sympathetic nervous system (activation response)
- Parasympathetic nervous system (recovery response)
The sympathetic branch prepares the body for action. As a result, heart rate increases. Alertness sharpens. Energy resources mobilize. In contrast, the parasympathetic branch promotes restoration. It slows physiological activity, supports digestion, and facilitates tissue repair.
Optimal neural regulation depends on sympathetic and parasympathetic balance. Regulation does not require constant calm. Instead, it requires the ability to activate when necessary and recover efficiently afterward.
Nervous System regulation vs Dysregulation
To understand Regulatory balance more clearly, it is helpful to examine its opposite state — dysregulation.
Regulation reflects adaptive flexibility. In contrast, dysregulation reflects prolonged imbalance.
In a regulated system:
- Stress responses activate appropriately
- Recovery cycles engage effectively
- Neural signaling remains proportionate
In a dysregulated system:
- Stress activation may persist chronically
- Recovery signaling may weaken
- Neural sensitivity may increase
Over time, dysregulation can influence inflammation patterns, pain perception, muscular guarding, and autonomic instability. Consequently, recovery environments may become less supportive. Consequently, nerve recovery environments may become less supportive, and repair processes may slow.

Why Nervous System regulation Matters in Nerve Recovery
Nerve healing does not occur in isolation. Instead, it depends heavily on the surrounding physiological environment. Instead, it depends heavily on the surrounding neural tissue environment.
When regulation remains stable, neural communication becomes more efficient and less reactive. As a result, the internal environment becomes more supportive of repair readiness.
- Blood flow improves
- Inflammatory signaling stabilizes
- Muscular compression reduces
- Cellular repair conditions strengthen
However, chronic dysregulation may elevate stress hormones, disrupt circulation patterns, and increase neural reactivity. As a result, recovery processes may slow or become inconsistent.
Understanding this relationship helps shift recovery thinking from symptom management toward systemic regulation support.
Factors Affecting Nervous System regulation
Nervous System regulation does not depend on a single biological process. Instead, it reflects the combined influence of psychological, physiological, metabolic, and environmental factors.
The nervous system continuously interprets internal and external signals to determine whether the body should remain in activation or restoration mode. Therefore, regulatory stability depends on how consistently the body receives signals of safety, energy sufficiency, and physiological balance.
When these inputs remain supportive, the nervous system balance strengthens. However, when stressors accumulate, adaptive flexibility may gradually decline.
Therefore, understanding regulatory stability becomes essential within nerve recovery education.
Stress & Emotional Load
Psychological stress is one of the most influential drivers of Nervous System regulation. The brain constantly evaluates emotional threat, uncertainty, and environmental pressure. As a result, stress activation pathways engage.
When stress perception increases, the sympathetic nervous system activates. This response prepares the body for action by elevating cortisol, increasing heart rate, and sharpening vigilance.
Short-term activation is adaptive. However, chronic emotional load can maintain prolonged activation states. As a result, parasympathetic recovery signaling may weaken.
Over time, this imbalance may influence:
- Neural sensitivity
- Muscular guarding
- Inflammatory signaling
- Pain perception patterns
Consequently, emotional regulation capacity becomes closely linked to nerve recovery environments.
Over time, this imbalance may influence neural sensitivity. Furthermore, it may increase muscular guarding and inflammatory signaling.
Sleep & Circadian Rhythm
Importantly, sleep plays a foundational role in nervous system regulation.
Sleep plays a foundational role during this phase in the nervous system’s balance. During restorative sleep cycles, the nervous system shifts toward parasympathetic dominance.
This state supports:
- Neural repair processes
- Neurotransmitter recalibration
- Inflammatory regulation
- Glymphatic detoxification activity
Circadian rhythm stability also supports regulatory balance. Consistent sleep–wake timing helps synchronize hormonal signaling, autonomic tone, and metabolic repair cycles.
Over time, circadian disruption may reduce regulatory adaptability and recovery efficiency.
However, disruption may elevate sympathetic activation. It may also reduce regulatory resilience, impair neural recovery readiness, and increase stress reactivity.
Therefore, sleep quality directly shapes regulatory capacity.

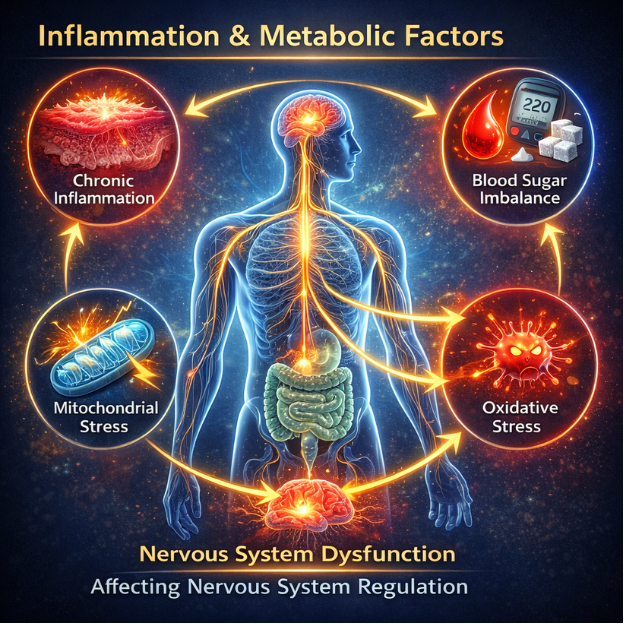
Inflammation & Metabolic Stability
Inflammatory signaling interacts closely with Nervous System regulation. The immune and nervous systems communicate continuously. They exchange signals through cytokines, neuropeptides, and stress hormones.
When inflammation remains acute and resolved, the regulatory balance typically remains intact. However, chronic low-grade inflammation may alter neural signaling thresholds.
Metabolic instability further compounds this effect. Consequently, neural signaling thresholds may shift. Fluctuating glucose levels, mitochondrial stress, and oxidative load can influence autonomic responsiveness and neural excitability.
Furthermore, metabolic strain can amplify inflammatory signaling pathways affecting neural responsiveness.
As a result, neural responsiveness may become more reactive under sustained metabolic strain.
This interaction highlights why systemic physiology influences neural recovery environments.
Role of Nervous System Regulation in Long-Term Nerve Recovery
Nervous System regulation shapes the internal conditions in which nerve repair occurs. It influences circulation patterns, inflammatory signaling, muscular tension, and cellular recovery readiness.
When regulatory balance remains stable:
- Blood flow to nerve tissue improves
- Oxygen delivery becomes more consistent
- Muscular compression decreases
- Repair signaling pathways strengthen
In contrast, chronic dysregulation may sustain stress activation, restrict circulation, and elevate neural irritability.
Over extended periods, these patterns can affect how efficiently nerves recover structural and functional stability.
Therefore, the regulatory function does not act as a therapy. Instead, it functions as a foundational biological environment that either supports or constrains long-term nerve recovery processes.
| Consequently, regulatory stability becomes essential for sustaining long-term recovery conditions. For this reason, regulatory balance becomes foundational within long-term nerve recovery. |
Biological Mechanisms of Nervous System Regulation
To understand this more clearly, the nervous system constantly interprets signals from the external environment.
Nervous System regulation operates through biological signaling networks. These networks coordinate communication between the brain and body. These mechanisms involve neurotransmitters, neurohormones, autonomic reflexes, and feedback loops.
The brain continuously interprets sensory input. It also processes emotional signals and physiological data. It then adjusts autonomic output through the hypothalamus and brainstem regulatory centers.
Key biochemical mediators include:
- Cortisol and stress hormones
- Adrenaline and noradrenaline
- Acetylcholine
- Serotonin and GABA
Balanced production and signaling of these mediators support the nervous system regulation. However, prolonged stress activation may disrupt neurotransmitter equilibrium and autonomic responsiveness.
Over time, this can alter neural excitability and regulatory stability.
Autonomic Flexibility & Vagal Tone
Autonomic Flexibility & Vagal Tone in Nervous System regulation
Autonomic flexibility refers to the nervous system’s ability to transition efficiently between activation and recovery states. It reflects how quickly the body can return to baseline after stress exposure.
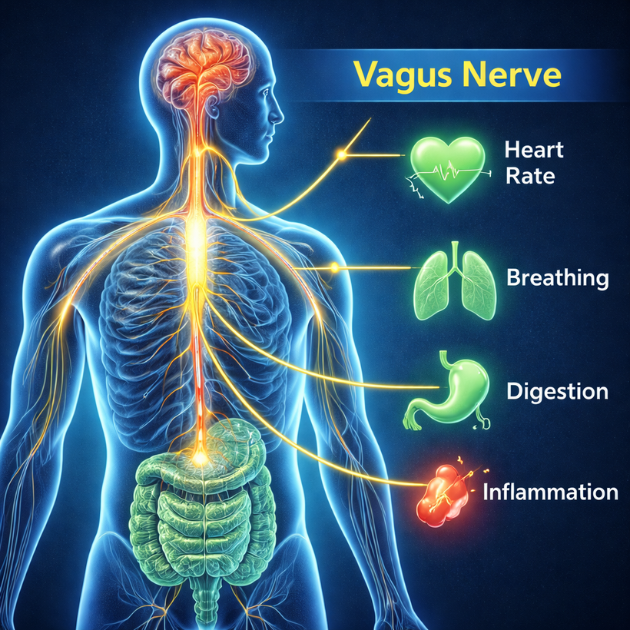
Vagal tone plays a central role in this process. The vagus nerve plays a central role in brain–body communication. Its broader vagus nerve function in the nervous system regulation includes influencing heart rate, breathing patterns, and digestive signaling.
Higher vagal tone is associated with:
- Improved heart rate variability patterns, reflecting stronger heart rate variability and regulation capacity
- Faster stress recovery
- Enhanced parasympathetic activation
- Better emotional regulation capacity
Lower vagal tone may reflect reduced regulatory adaptability and prolonged sympathetic dominance.
Therefore, vagal signaling strength becomes a measurable indicator of regulatory capacity.
Adaptation Capacity Within Nervous System Regulation
Adaptation capacity describes how the nervous system adjusts to repeated stimuli over time. This includes both physiological and psychological stress exposure.
When adaptive capacity remains strong, the nervous system learns to differentiate between threat and safety more efficiently. As a result, activation responses become proportionate rather than excessive.
However, chronic overload may narrow this adaptive window. The system may begin responding defensively to low-level stimuli, increasing neural sensitivity and stress reactivity.
This phenomenon explains why dysregulation can persist even after the original stressor resolves.

Environmental Safety Signaling and Nervous System Regulation
The nervous system constantly scans the environment for cues of safety or threat. This process occurs subconsciously through
neuroception and safety signaling — the brain’s automatic threat detection system.
In this context, the nervous system constantly scans the environment for cues of safety or threat.
Safety signals may include:
- Predictable environments
- Supportive social interaction
- Emotional stability
- Physiological comfort
Threat signals may include:
- Chronic uncertainty
- Pain or inflammation
- Sleep deprivation
- Emotional distress
| When safety signaling predominates, parasympathetic activation strengthens. As a result, regulatory stability improves, and recovery signaling becomes more supportive. As a result, parasympathetic activation strengthens when safety signaling predominates. |
Education-Based Support Layers for Nervous System Regulation
This module maintains an education-focused, non-protocol framework. Therefore, rather than prescribing interventions, it introduces conceptual support layers that influence the nervous system regulation.
Awareness & Signal Interpretation
Understanding how stress, emotion, and physiology influence neural signaling builds regulatory awareness. Education reduces uncertainty and reframes threat perception.
Behavioral Rhythm Stability
Consistent daily rhythms support autonomic predictability. Stable sleep timing, activity cycles, and recovery periods influence regulatory signaling patterns.
Emotional Processing Capacity
Emotional suppression or overload can influence autonomic tone. Education around emotional processing helps contextualize stress responses.
Physiological Resource Availability
Energy sufficiency, metabolic stability, and inflammatory balance shape how resilient regulatory systems remain under stress.
Integration of Nervous System Regulation Within the Nerve Recovery Framework
Nervous System regulation does not function as an isolated recovery element. Instead, it integrates with multiple biological systems that collectively shape the internal healing environment.
- Circulation and oxygenation
- Inflammatory regulation
- Repair nutrition
- Muscular environment
- Sleep physiology
This systems-based interaction explains why regulatory stability is foundational for long-term nerve recovery education. It highlights that recovery readiness depends on interconnected biological conditions rather than single-factor influence.
Together, these interconnected systems shape the broader biological environment supporting nerve recovery.
Related Learning: