Free Nerve Healing Guide: Understanding Nerve Health & Recovery
This free guide is designed to help you understand nerve health through calm, structured, education-first learning. This nerve healing guide was created to provide a structured, education-first understanding of nerve health, damage, and recovery. Rather than offering quick fixes, it explains how biological systems influence nerve function over time — helping you build clarity, reduce confusion, and navigate recovery learning with confidence. active Heading
Calm Orientation of This Guide
Understanding nerve health can often feel overwhelming. Many people encounter fragmented information, conflicting advice, and overly technical explanations that increase confusion rather than reduce it. For this reason, this free guide was created as a structured, education-first resource to simplify understanding of nerve function, damage, and recovery.
Understanding the Purpose of This Guide
This guide is intended for individuals who want clarity — not quick fixes. Whether you are experiencing nerve discomfort, supporting someone in recovery, or simply trying to understand how the nervous system responds to stress and biological strain, this resource provides a calm and organized learning foundation.
What This Guide Is and Is Not
Importantly, this guide does not function as a treatment manual or medical directive. Instead, it focuses on biological education. By explaining how nerves operate, how dysfunction develops, and how recovery environments are supported, it helps readers build system-level understanding rather than relying on isolated tips.
In addition, structured knowledge reduces unnecessary fear. When people understand what is happening inside the body, uncertainty often decreases. As a result, they are better able to navigate recovery conversations, lifestyle adjustments, and long-term health decisions with greater confidence.
What You Will Gain From Structured Learning
Throughout this guide, you will learn how multiple systems — including inflammation pathways, metabolic balance, nervous system regulation, and repair biology — interact to influence nerve health. More importantly, you will see how these systems connect within a broader recovery framework.
Before moving forward, it is helpful to remember that recovery timelines vary, biological responses differ, and education plays a critical role in reducing confusion. This guide serves as your starting orientation within that structured learning journey.
This nerve healing guide serves as your structured starting point for understanding recovery systems.
Why Nerve Damage Happens — A Nerve Healing Guide Perspective
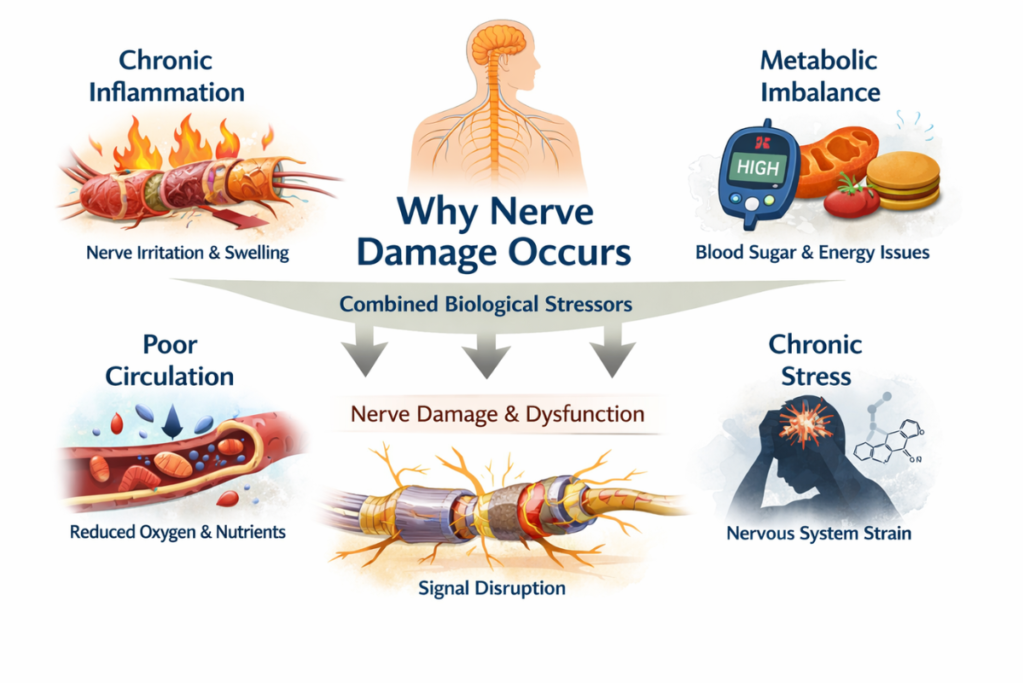
In this nerve healing guide, understanding why nerve damage develops forms the foundation of recovery education.
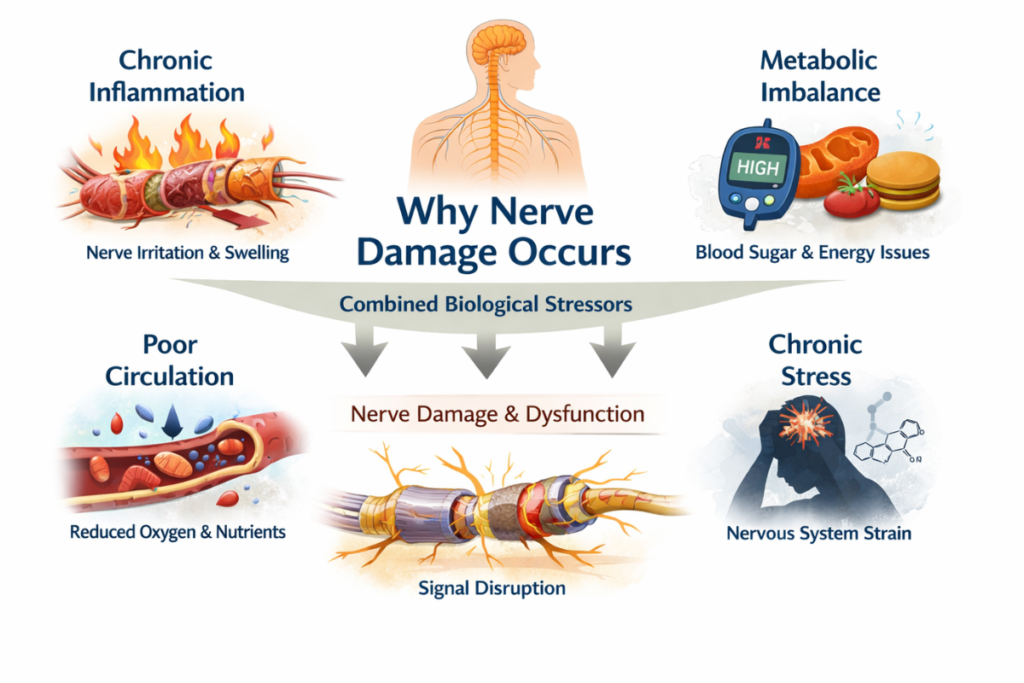
Nerve damage rarely develops from a single isolated cause within broader biological stress systems. Instead, it often emerges gradually through a combination of biological stressors that affect how nerves function, communicate, and repair over time. Understanding these underlying mechanisms is essential because it shifts the focus from surface symptoms to deeper physiological processes.
How Nerves Function as Communication Pathways
To begin, nerves function as communication pathways. They transmit electrical and chemical signals between the brain, spinal cord, and the rest of the body. These signals regulate sensation, movement, organ activity, and protective reflexes. When nerve structures remain intact, signal transmission flows efficiently. However, when structural or biochemical disruptions occur, communication becomes impaired.
The Role of Inflammation and Oxidative Stress
One foundational factor involves chronic inflammatory signaling pathways. When inflammatory pathways remain chronically activated, they can irritate nerve fibers and surrounding tissues. Over time, this inflammatory pressure may interfere with signal conduction, contributing to sensations such as tingling, burning, or numbness. In addition, oxidative stress can further strain nerve cells by damaging cellular components essential for signaling stability.
Metabolic and Circulatory Influences
Metabolic dysfunction processes within systemic metabolic repair systems also play a significant role. Nerve tissue is metabolically demanding, meaning it requires a consistent energy supply to maintain function and repair capacity. When blood sugar instability, mitochondrial dysfunction, or nutrient transport issues develop, nerves may struggle to sustain signaling efficiency. As a result, functional decline can occur gradually rather than suddenly.
Circulatory support systems within microvascular recovery networks represent another critical dimension. Peripheral nerves depend on oxygen and nutrient delivery through microvascular blood flow. If circulation becomes compromised, nerve tissues may experience reduced oxygenation. Over time, this can weaken structural integrity and slow repair processes.
Chronic Stress and Nervous System Overload
Nervous system regulation balance within autonomic regulation frameworks further compounds these biological pressures. When the nervous system remains in prolonged activation states, regulatory balance can shift. Stress hormones, autonomic dysregulation, and systemic inflammation may interact to increase neurological strain. Consequently, nerve resilience may decrease while symptom sensitivity increases.
It is also important to recognize that nerve dysfunction often progresses slowly. Early changes may be subtle and intermittent. However, as multiple stressors accumulate — inflammatory, metabolic, circulatory, and neurological — functional disruption becomes more noticeable.
By understanding how these mechanisms interact, readers can begin to see nerve damage not as a sudden event, but as a systems-based process influenced by internal biological environments. This perspective creates a more realistic foundation for exploring recovery and regeneration in the sections that follow.
This systems-based perspective, outlined throughout the nerve healing guide, reframes how dysfunction is understood.
Ready to Understand How Recovery Begins?
Explore the structured learning pathway that explains how regulation, repair, and recovery systems work together over time.
The Biological Systems Explained in This Nerve Healing Guide
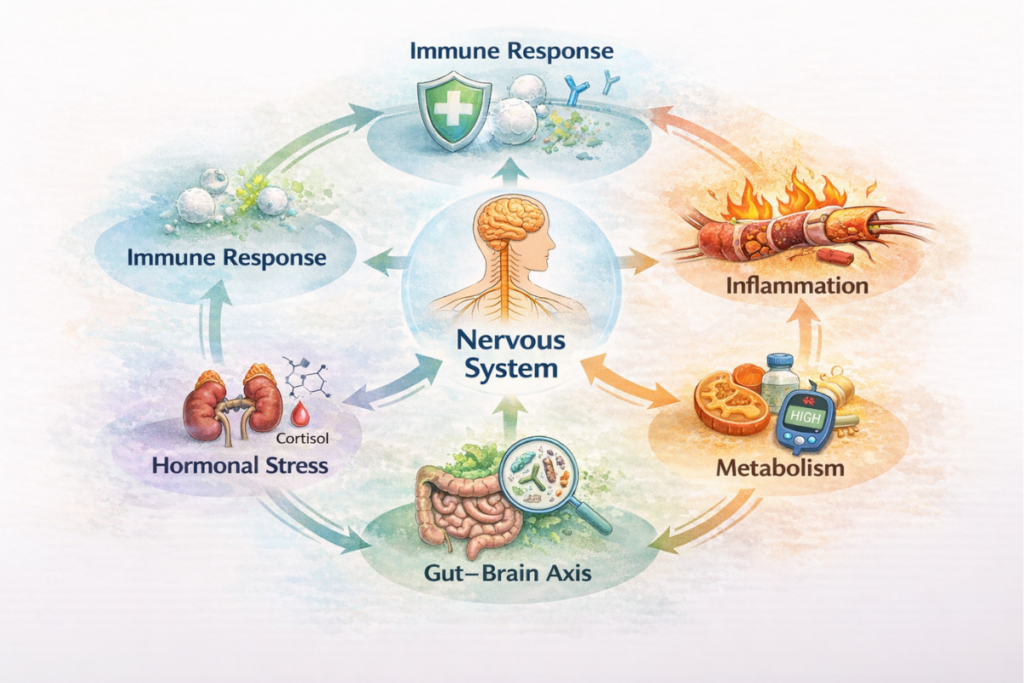
Nerve dysfunction rarely develops in isolation. Instead, it reflects the interaction of multiple biological systems that collectively influence how nerves function, adapt, and recover. Understanding these interconnected systems provides a deeper perspective by revealing why nerve health cannot be explained by a single pathway.
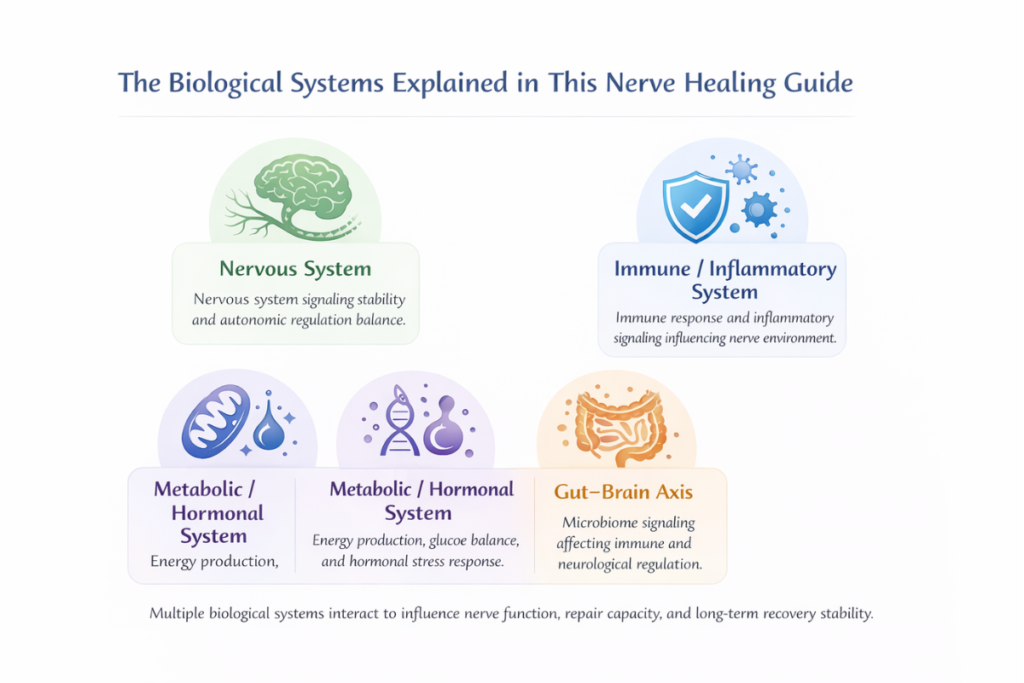
Nervous System Regulation
To begin, nervous system regulation capacity plays a central role. The autonomic nervous system continuously balances activation and recovery states. When this regulatory capacity becomes strained — often due to prolonged stress exposure — signaling stability may decline. As a result, nerves can become more reactive, sensitive, or energetically depleted over time.
Immune and Inflammatory Interaction
In addition, the immune and inflammatory response contributes significantly to nerve health. Immune activation is essential for protection and repair. However, when inflammatory pathways remain chronically elevated, they may begin to influence nerve tissues indirectly. Persistent inflammatory signaling can create an environment where nerve irritation, swelling, and functional disruption become more likely.
These neuroimmune interaction systems play a central role in long-term inflammatory regulation.
Metabolic and Hormonal Balance
Metabolic repair systems represent another foundational pillar. Nerve cells require consistent energy production to maintain electrical signaling and cellular repair. Mitochondria — the energy generators within cells — support this process. When metabolic instability develops, whether through glucose dysregulation or impaired nutrient utilization, nerve resilience may gradually weaken.
Hormonal stress responses further shape this landscape. Stress hormones, particularly when elevated for extended periods, can influence inflammation levels, metabolic function, and nervous system tone simultaneously. Consequently, long-term stress exposure often produces system-wide effects rather than localized ones.
Gut–Nerve Communication
The gut–brain axis communication also deserves attention. The gut microbiome influences immune signaling, inflammatory modulation, and nutrient absorption. Because these systems are biologically linked, disturbances within gut ecology may indirectly affect nerve stability and repair capacity.
When viewed together, these systems form an interaction model rather than independent pathways. Nervous system regulation, immune activity, metabolic function, hormonal signaling, and gut health continuously communicate. Therefore, nerve dysfunction often reflects cumulative strain across these domains rather than a singular cause.
By recognizing this multi-system framework, readers can better understand why recovery education emphasizes systemic balance. This perspective prepares the foundation for exploring how regeneration and repair mechanisms operate within supportive biological environments.
Within this nerve healing guide, these interconnected systems are explained as a unified biological model.
How Nerve Recovery Works in a Structured Nerve Healing Guide
This nerve healing guide explains regeneration as a gradual biological process rather than an instant repair event.
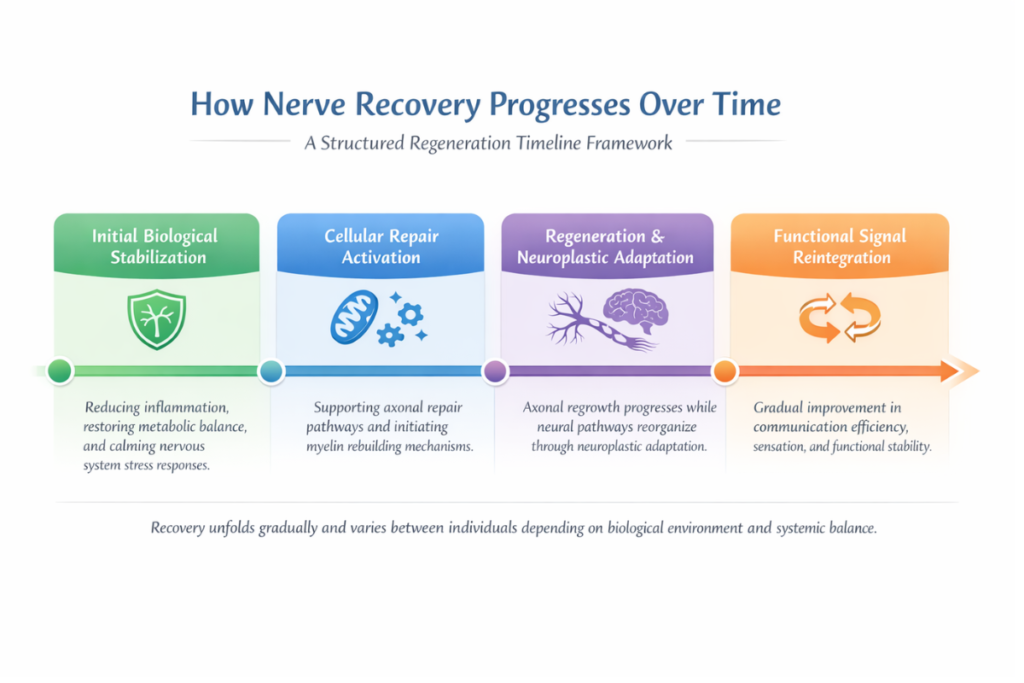
Nerve recovery is often misunderstood as a rapid or linear process. In reality, regeneration occurs gradually through complex biological repair mechanisms that unfold over time. Understanding how this process works helps establish realistic expectations while reducing unnecessary frustration during recovery phases.
To begin, nerves possess an inherent capacity for repair. Peripheral nerves, in particular, can regenerate under supportive biological conditions. However, this repair does not occur instantly. Instead, it involves coordinated cellular activity aimed at restoring structural integrity and functional signaling pathways.
Axonal Regeneration Mechanisms
One of the central processes involved is the axonal regeneration mechanism within structured nerve regrowth systems. The axon — the long fiber responsible for transmitting electrical signals — may begin to regrow when damage occurs. This regrowth follows a slow, guided pathway. In many cases, supportive cells create structural channels that help direct regenerating nerve fibers toward their original targets. As a result, signal restoration may gradually improve as structural continuity is re-established.
Myelin Repair and Signal Restoration
In addition to axonal repair, myelin repair processes play a critical role. Myelin is the protective sheath that surrounds nerve fibers and facilitates efficient signal transmission. When myelin becomes compromised, electrical conduction may slow or destabilize. Over time, remyelination processes can help restore signal efficiency, although this, too, depends on supportive biological conditions.
Neuroplasticity and Functional Adaptation
Neuroplastic adaptation introduces another dimension to recovery. The nervous system is capable of adapting its signaling pathways in response to injury or functional disruption. Through neuroplastic changes, the brain and peripheral nerves may reorganize communication routes to compensate for damaged areas. Consequently, functional improvements may emerge even when structural repair remains incomplete.
Time remains one of the most influential variables in nerve regeneration. Unlike tissues with rapid turnover, nerve repair progresses slowly. Biological rebuilding, signal recalibration, and structural stabilization require sustained physiological support. Therefore, gradual change is often more realistic than immediate restoration.
Environmental Factors Influencing Recovery
The recovery-supportive biological environment also influences recovery capacity. Inflammatory balance, metabolic stability, circulation quality, and nervous system regulation all contribute to repair readiness. When these supportive conditions are present, regenerative processes may operate more efficiently.
Because multiple mechanisms operate simultaneously — structural repair, myelin restoration, neuroplastic adaptation, and environmental stabilization — nerve recovery reflects a systems-based progression rather than a single event. This perspective reinforces the importance of understanding recovery as a coordinated biological process shaped by time, environment, and systemic balance.
Explore the Systems That Support Recovery
Dive deeper into the biological repair systems, regeneration pathways, and recovery engineering frameworks that guide long-term education on nerve healing.
In the next section, we explore the stabilizing factors that help sustain these regenerative processes and support long-term healing capacity.
As discussed in this nerve healing guide, neuroplasticity supports functional adaptation during recovery.
Stabilizing Factors Within a Nerve Healing Guide Framework
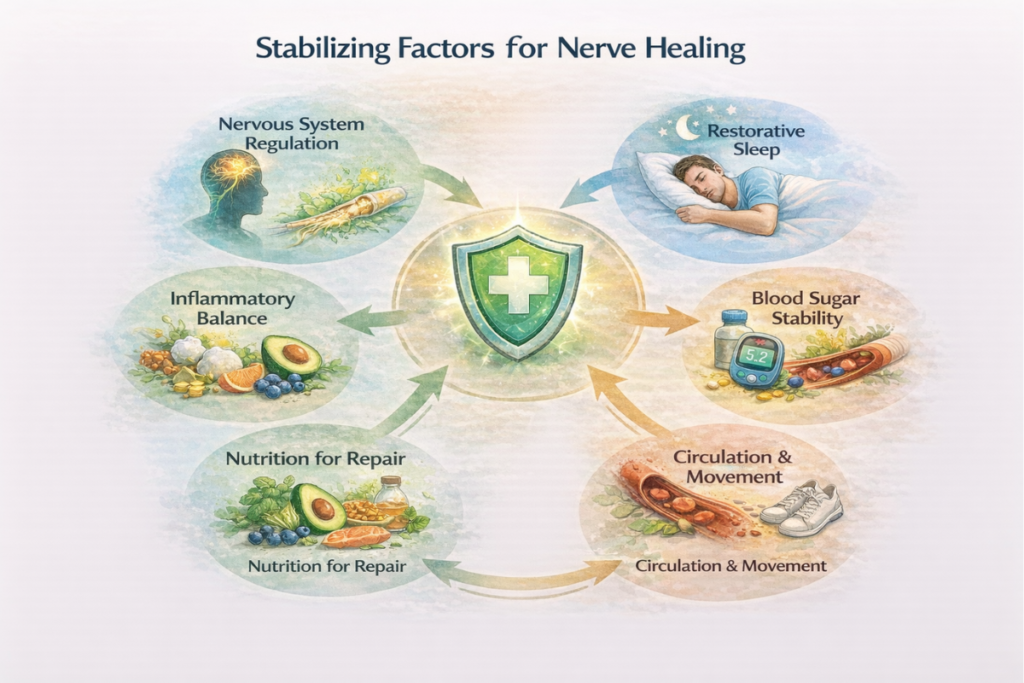
While nerve regeneration involves structural repair and neurological adaptation, recovery does not depend on regeneration alone. Instead, it is strongly influenced by the biological environment in which healing takes place. Stabilizing this internal environment helps create conditions where repair processes can operate more effectively over time.
Nervous System Regulation Stability
One of the most influential stabilizing factors is nervous system regulation stability. When the autonomic nervous system maintains balance between activation and recovery states, physiological strain is reduced. However, when stress responses remain chronically elevated, repair resources may be diverted toward survival signaling rather than restoration. As a result, healing efficiency can become compromised.
Sleep and Biological Repair Cycles
Restorative sleep cycles also play a foundational role in stabilization. During restorative sleep cycles, the body engages in cellular repair, inflammatory modulation, and neurological recalibration. In addition, sleep supports hormonal balance and metabolic regulation — both of which contribute to nerve recovery readiness. When sleep quality declines, these repair processes may become less efficient.
Metabolic and Nutritional Foundations
Metabolic blood sugar balance represents another critical dimension. Nerve cells rely on a consistent energy supply to maintain signaling and structural maintenance. When glucose levels fluctuate significantly, metabolic stress may increase. Over time, this instability can influence inflammation levels, mitochondrial function, and overall nerve resilience.
Inflammation Balance and Repair Readiness
Inflammation regulation systems remain equally important. While acute inflammation supports repair, chronic inflammatory activation can create an environment that strains nerve tissues. Therefore, maintaining inflammatory equilibrium helps protect structural integrity while supporting regenerative pathways.
Nutritional repair foundations also contribute to stabilization. Nerve tissue requires micronutrients, fatty acids, and metabolic cofactors to sustain cellular repair and signaling stability. Rather than focusing on isolated nutrients, the broader nutritional environment influences how effectively repair processes unfold.
Movement, Circulation, and Stress Balance
Circulatory support mechanisms further enhance stabilization. Gentle physical activity promotes blood flow, oxygen delivery, and metabolic exchange. Consequently, improved circulation may help sustain the biological conditions required for repair and regeneration.
Stress reduction completes this stabilizing framework. Because chronic stress influences inflammation, hormonal signaling, and nervous system regulation simultaneously, reducing stress load can positively affect multiple recovery pathways at once.
Taken together, these stabilizing factors — regulation, sleep, metabolic balance, inflammation control, nutrition, circulation, and stress modulation — create the environmental foundation that supports nerve healing capacity. In the next section, we shift from stabilization to long-term protection, exploring how sustained balance helps reduce relapse risk and protect recovery progress over time.
Learn How to Protect Recovery Progress
Discover how long-term protection strategies, relapse prevention systems, and lifestyle stabilization frameworks help sustain nerve recovery over time.
Long-Term Protection in a Comprehensive Nerve Healing Guide
Nerve recovery does not end when symptoms begin to improve. In many cases, long-term protection becomes just as important as initial stabilization and regeneration. Without sustained balance, the same biological stressors that contributed to dysfunction may gradually re-emerge. Therefore, understanding relapse prevention requires a systems-based mindset rather than a short-term solution.
Understanding Relapse Risk
To begin, relapse risk often develops when underlying stressors return unnoticed. For example, chronic inflammation and metabolic instability, sleep disruption, or prolonged stress exposure may slowly accumulate again. Over time, these pressures can recreate the internal environment that previously strained nerve function. Consequently, maintenance becomes a proactive process rather than a reactive one.
The Impact of Chronic Stress Load
Chronic stress regulation patterns deserve particular attention. Even when structural repair has progressed, persistent autonomic activation may continue to influence inflammation and hormonal balance. As a result, nervous system regulation remains a long-term priority. Sustaining recovery requires ongoing attention to how the body transitions between activation and rest states.
Lifestyle drift is another common factor. After improvement occurs, routines may gradually shift. Sleep schedules become inconsistent, nutritional patterns fluctuate, and stress management practices decline. Although these changes may seem minor at first, their cumulative impact can influence biological stability over months or years.
Protective Routines and System Maintenance
Structured recovery maintenance routines help counter this drift. Consistent sleep timing, balanced nutrition, regular movement, and stress modulation practices create a stabilizing rhythm. In addition, periodic self-awareness regarding energy levels, sensation changes, and stress patterns allows earlier detection of imbalance. Early awareness often supports faster course correction.
System maintenance thinking shifts recovery from a temporary effort to a sustainable practice. Instead of focusing solely on symptom relief, individuals can view nerve health as part of broader biological regulation. This perspective reinforces long-term resilience rather than short-term reaction.
Building Long-Term Resilience
Resilience building also involves adaptability. Because biological responses differ between individuals, protection strategies must remain flexible. What stabilizes one system at a particular time may require adjustment later. Therefore, education continues to play a central role in long-term protection.
Ultimately, long-term protection is not about eliminating all stressors. Instead, it is about maintaining sufficient systemic balance so that nerve tissues remain supported despite normal life fluctuations. In the final section, we will explore how to continue this structured learning journey through the broader education pathways available within this guide.
Continuing Your Structured Learning Journey
By this point, you have explored how nerve dysfunction develops, how regeneration occurs, and which stabilizing factors support long-term protection. However, understanding these foundations is only the beginning. Sustainable progress often depends on continuing structured learning rather than relying on isolated pieces of information.
Expanding Beyond Foundational Knowledge
This nerve healing guide serves as an orientation layer within a broader educational framework. It introduces the core biological systems involved in nerve health. Now, the next step is to deepen that understanding through focused pathways that explore specific mechanisms in greater detail.
Exploring the Structured Learning Path
For example, the Learning Path section expands on nervous system regulation, repair nutrition, inflammation balance, and recovery engineering in a step-by-step progression. Instead of presenting scattered topics, it organizes information in a logical sequence. As a result, readers can move forward without feeling overwhelmed.
Condition-Focused Education Pathways
In addition, the Conditions section provides context-specific education related to common nerve-related concerns. While this guide explains foundational principles, condition-focused pages help clarify how those principles apply in different biological scenarios. Therefore, readers can explore topics relevant to their own experiences while maintaining a systems-based perspective.
Importantly, structured progression reduces confusion. When information is consumed in a deliberate order, concepts connect more clearly. Consequently, recovery education becomes less fragmented and more actionable from a learning standpoint.
As you continue, remember that recovery timelines vary and biological responses differ between individuals. Education does not replace medical care. Instead, it supports informed conversations and a clearer understanding of how the nervous system functions over time.
Navigating Your Next Steps
You may now choose to:
- Begin the full Learning Path for step-by-step, structured education
- Explore Conditions to understand specific nerve-related topics
- Revisit earlier sections of this guide to reinforce foundational concepts
Each pathway builds upon the principles introduced here. By progressing calmly and systematically, you strengthen not only your understanding but also your long-term resilience.
This concludes the orientation layer of the nerve healing guide. The next phase of your journey continues within the broader learning system designed to support clarity, structure, and sustainable nerve health education.
Continue Your Structured Nerve Healing Education
Choose your next learning pathway to deepen your understanding of nerve recovery systems, biological stabilization, and long-term healing frameworks.